Trigger finger
Trigger finger (or trigger thumb) is a condition where your digit catches, snaps, or becomes stuck when you try to bend or straighten it. This clicking or locking sensation occurs as the tendon struggles to glide smoothly through its sheath.
Why does it happen?
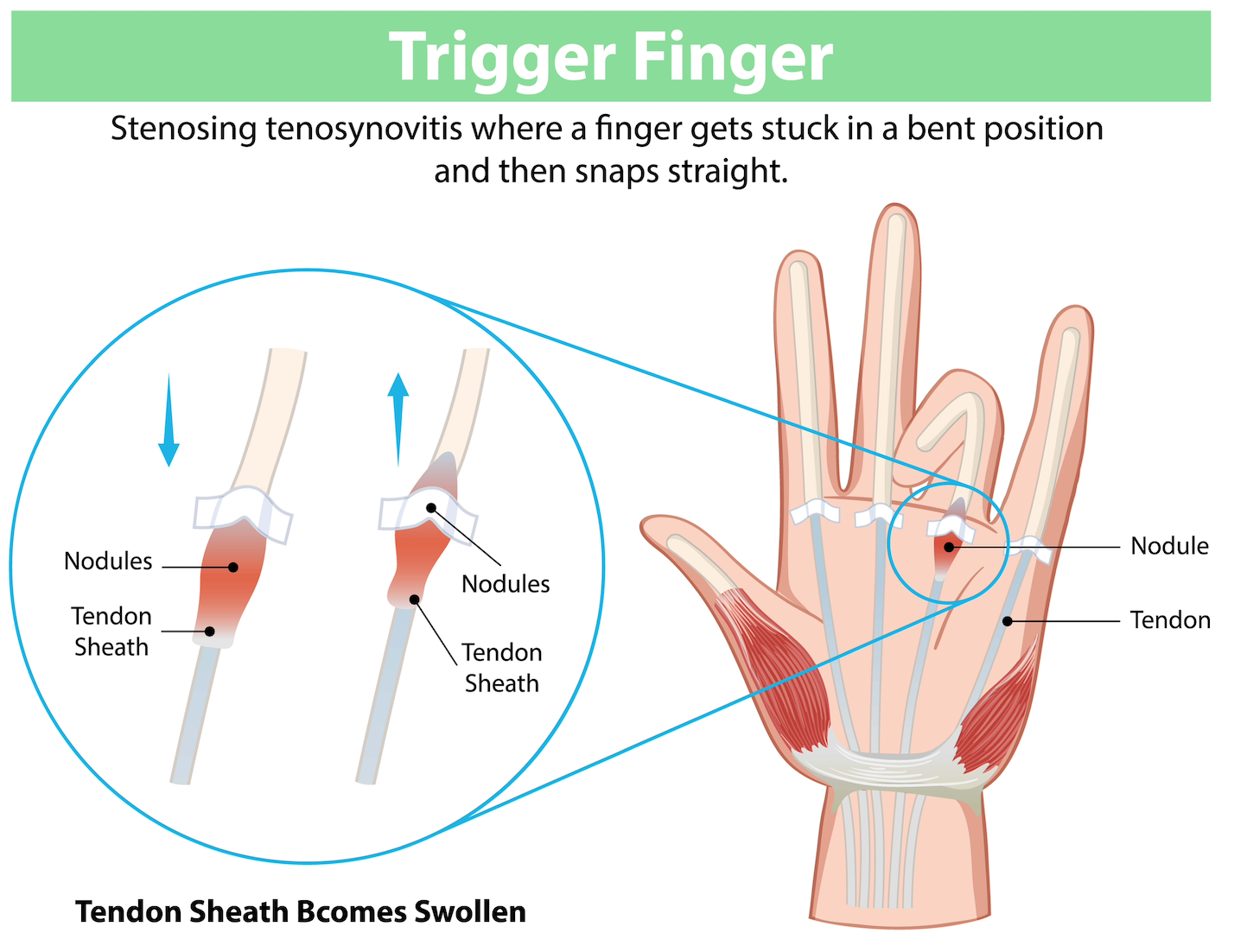
The flexor tendons in your fingers run through narrow tunnels called pulleys. When the entrance to one of these tunnels becomes thickened or swollen, the tendon's surface can become irregular. This creates friction, causing the tendon to catch as it tries to pass through.
While trigger finger can affect anyone, certain factors increase risk. People with insulin-dependent diabetes are particularly susceptible. Sometimes triggering develops after direct trauma to the palm, though most cases arise without obvious injury. In patients with rheumatoid arthritis, nodules on the tendon itself may cause triggering.
There's limited evidence linking trigger finger to occupational activities, though symptoms are often aggravated by repetitive hand use - whether at work, during household tasks, gardening, or sports. Importantly, this condition is not related to osteoarthritis.
-
Discomfort in your palm where the finger joins the hand, or at the thumb's middle joint
Tenderness when pressing the affected area
Catching or snapping sensation during finger movement
The digit locking in a flexed position, particularly noticeable upon waking
Needing to use your other hand to straighten the affected finger
Joint stiffness (especially common in trigger thumb affecting the tip joint)
Typically affects people over 40 years old
-
While trigger finger can be frustrating and uncomfortable, it's not dangerous. Mild cases sometimes resolve spontaneously within several weeks. Treatment choices include:
Activity modification
When feasible, reducing activities that provoke symptoms can allow natural improvement.
Night splinting
Wearing a splint that keeps your finger straight overnight can be effective. A hand therapist can fabricate a custom splint. Keeping the tendon extended through the night allows the irregular segment to smooth out.
Corticosteroid injection
Injections successfully resolve symptoms in approximately 70% of patients, though effectiveness is somewhat lower in diabetic individuals. Side effects are uncommon but may include minor skin changes or pigmentation alteration at the injection site. Relief might begin within days or take several weeks to manifest. Occasionally a second injection proves beneficial, though persistent triggering may warrant surgical consideration.
-
Surgery involves widening the tendon tunnel by dividing its constraining roof (releasing the A1 pulley). The procedure can be performed under local anaesthesia (numbing just the surgical site), regional nerve block (numbing your entire arm), or general anaesthesia.
Through a small incision, I carefully release the tunnel while protecting nearby nerves. You'll need a light dressing for 10-14 days. Gentle hand use is encouraged from day one, and active finger movement actually promotes recovery. Pain typically resolves quickly. The scar may feel firm and appear pink for some weeks but rarely causes long-term issues. Recurrence after surgery is unusual.
