Base of thumb arthritis
Understanding the condition
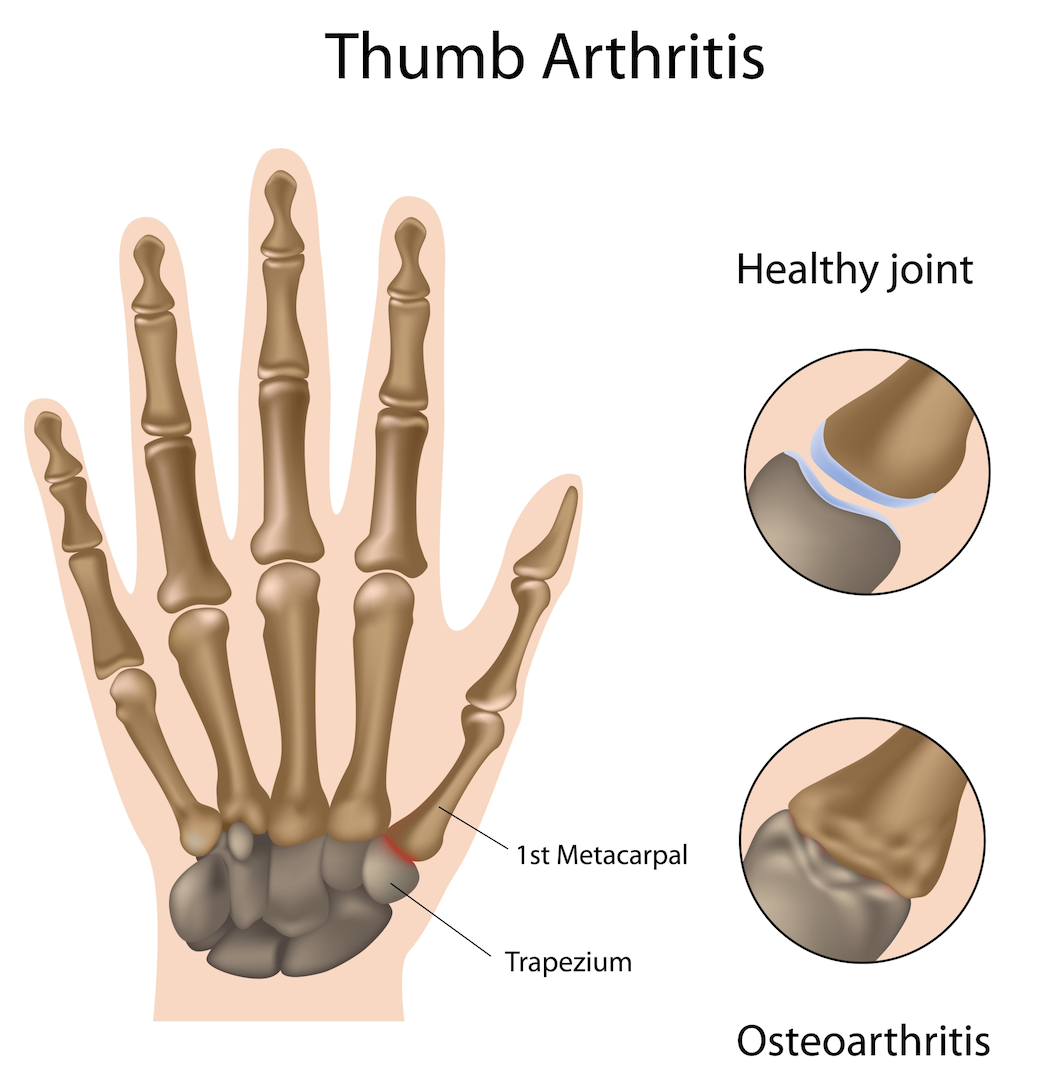
The carpometacarpal (CMC) joint at your thumb's base - where the metacarpal meets the trapezium bone - commonly develops osteoarthritis with aging. This saddle-shaped joint is responsible for the thumb's remarkable mobility but becomes susceptible to cartilage wear over time.
Osteoarthritis involves progressive deterioration of the smooth cartilage coating bone surfaces within joints. As cartilage thins and roughens, exposed bone ends generate friction and discomfort. While onset can occur at any age, symptoms typically emerge after 45 years. Familial tendency exists, and previous fractures or dislocations involving this joint may predispose to later arthritic changes.
This condition predominantly affects women - radiographic studies reveal its presence in approximately 25% of women beyond age 55, though substantially fewer men develop it. Notably, many individuals with radiographic arthritis remain asymptomatic or experience only minor discomfort.
-
Aching localised to the thumb base, worsened by pinching or gripping activities
Tenderness upon direct pressure over the joint
Functional challenges with tasks requiring forceful thumb use (jar opening, key turning, door knobs)
Diminished thumb mobility and reduced ability to spread the thumb away from the palm
In advanced disease, a prominent bump develops at the thumb base, and the middle thumb joint may compensate by hyperextending, creating a characteristic Z-shaped profile
-
Conservative approaches often provide adequate symptom control:
Activity modification: avoiding provocative movements allows symptom settling.
Medications: oral analgesics and anti-inflammatory drugs help manage discomfort. Your pharmacist or GP can recommend appropriate options.
Orthotic support: thumb spica splints provide mechanical unloading. Rigid constructs (metal or thermoplastic) offer maximum support but limit function. Flexible neoprene sleeves represent a more practical compromise for daily activities.
Corticosteroid injections: injections frequently reduce pain, though benefits may diminish over time. Side effects are uncommon but occasionally include skin changes at the injection site (such as loss of pigmentation). Relief might begin within days or require several weeks to manifest. Repeat injections are possible if needed.
-
Surgery represents a final option since symptoms often plateau and respond to conservative measures. When surgical treatment becomes necessary, several techniques exist:
Osteotomy: realigning the metacarpal bone adjacent to the arthritic joint. This procedure is reserved for early arthritis where only part of the joint is affected.
Trapeziectomy: removing the trapezium bone (one arthritic surface), sometimes combined with ligament reconstruction using tendon grafts
Arthrodesis: fusing the joint to eliminate motion and pain
Arthroplasty: joint replacement with prosthetic implants
Denervation: dividing small sensory nerve branches transmitting pain signals from the joint
Trapeziectomy remains the most frequently performed procedure for this condition. I'll discuss which approach best suits your individual circumstances and symptom pattern.
