Nail bed injuries
Understanding nail bed injuries
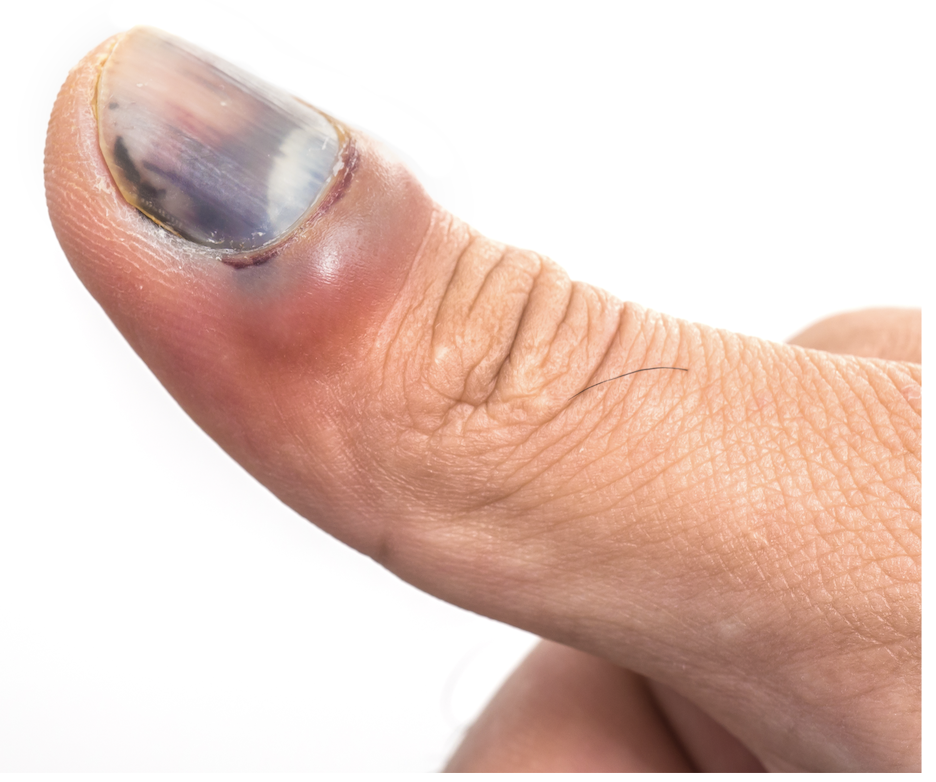
The nail bed comprises the tissue beneath your fingernail. Injuries to this area range in severity from subungual haematomas (blood accumulation causing dark discolouration beneath the nail) to partial or complete nail avulsion, lacerations extending through the nail plate and potentially involving bone fractures, through to near-complete fingertip amputations.
Common injury mechanisms include fingers caught in closing doors (particularly frequent in children) and accidents involving tools causing crushing or cutting trauma.
-
Management goals include wound decontamination to prevent infection, restoration of soft tissue and skeletal structures, and wound closure to facilitate healing.
Immediate first aid
Irrigate the wound under running tap water immediately. Take oral analgesics promptly - this makes subsequent care (dressing application, examination) more tolerable. Apply gentle sustained pressure with hand elevation to control bleeding.
When to seek medical attention
Minor injuries (simple crush without significant disruption) may heal spontaneously over several weeks without intervention. More significant injuries warrant professional assessment.
Medical management
Healthcare providers will thoroughly irrigate and dress the wound. Radiographs confirm suspected fractures.
In adults and older children, digital nerve blocks (local anaesthetic injections) allow comfortable repair. Younger children require general anaesthesia for surgical treatment. Most fingertip fractures require washing out and soft tissue repair only, but comminuted or displaced fractures may need wire or pin fixation for stability
-
Initial dressing changes typically occur around 10 to 14 days post-injury. Antibiotics aren't routinely indicated but may be prescribed for contaminated or extensive injuries.
Simple injuries may need only a single follow-up visit, while complex cases require multiple appointments. Serial radiographs may monitor fracture healing. Wire fixation sometimes requires secondary removal procedures - wires left protruding through the skin can be extracted easily in clinic without anaesthesia.
Maintaining mobility in uninjured finger joints is crucial to prevent stiffness. Scar massage and desensitisation exercises are useful and, occasionally, formal hand therapy becomes necessary.
-
Outcomes are generally excellent, particularly in paediatric patients. If your nail was removed during repair, expect regeneration over approximately three to six months. The emerging nail often appears thickened and irregular initially but typically normalises over time. Permanent nail deformity is uncommon.
Discomfort usually resolves within two weeks, though mild cold-weather sensitivity may persist. Initial stiffness typically improves with normal hand use.
-
Infection: Uncommon but characterised by increasing warmth, erythema, and pain. Seek prompt evaluation if these develop - oral antibiotics usually suffice for treatment.
Tissue necrosis: Rarely, severely traumatised tissue fails to survive, becoming infected or progressively necrotic (blackened). Additional surgery may be required to debride non-viable tissue.
