Hand fractures
What is a hand fracture?
Your hand contains numerous bones. When one breaks, the injury can range from a clean split creating two fragments to a shattered bone with many pieces. The overlying skin may remain unbroken (closed injury) or rupture to expose the underlying fracture (open injury).
Complexity increases when the fracture line runs through a joint's articulating surface or when surrounding structures like tendons, nerves, or vessels sustain concurrent damage.
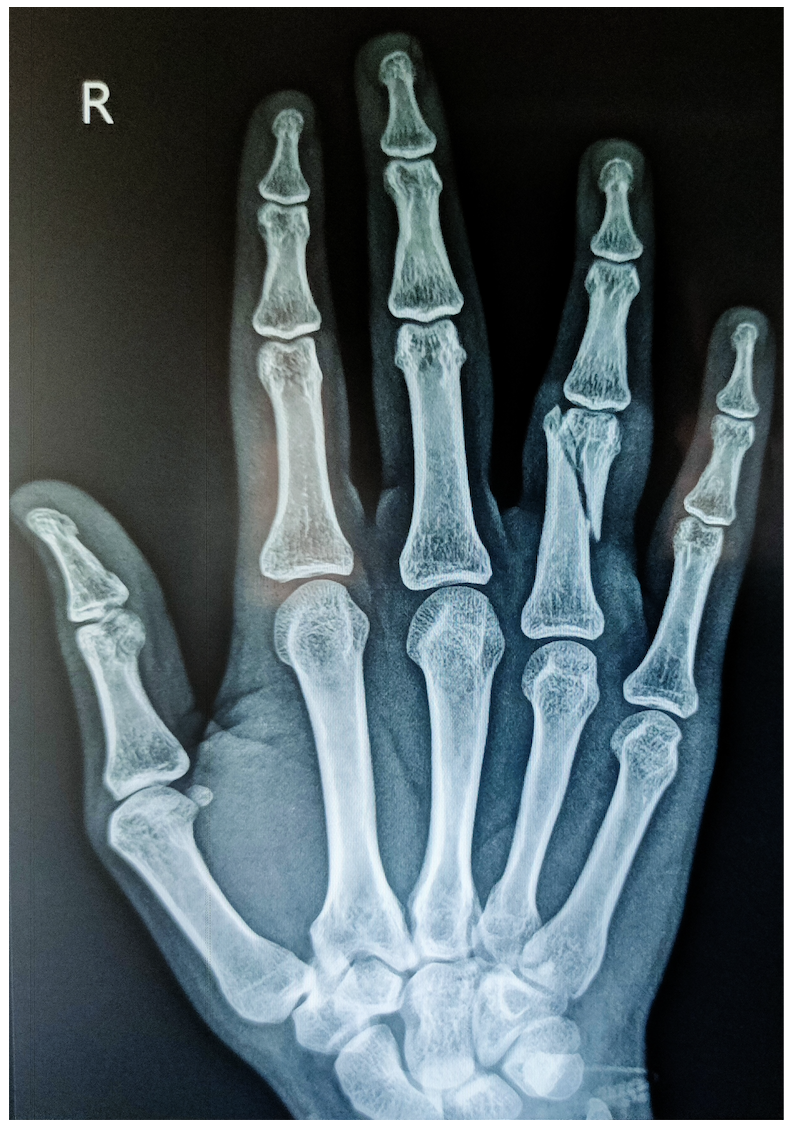
-
Bones break when subjected to force beyond their tolerance threshold. The fracture's anatomical position and configuration tell a story about the forces involved, making your description of events clinically valuable. I encourage honesty about circumstances regardless of how the injury happened - this information genuinely influences management decisions.
Typical scenarios include:
Trips and falls
Athletic trauma
Compression injuries
Traffic collisions
Physical altercations
-
Typical symptoms include:
Pain and swelling
Bruising
Reduced ability to move your fingers or thumb
Visible deformity of the digits
Numbness or tingling sensations
A wound (in open fractures)
-
If you think you've fractured your hand:
Remove all finger rings and jewellery without delay
Elevate your hand (higher than your elbow)
Apply clean covering to any breaks in skin
Obtain medical assessment at an emergency facility or general practice
-
My objective is optimising your hand's functional recovery.
Clinical evaluation
Assessment begins with clinical examination and radiographic imaging. Multiple variables shape the treatment blueprint: the affected bone's identity, where along its length the break occurred, degree of malalignment, whether single or multiple bones fractured, presence of additional trauma, which hand you primarily use, your work requirements, and existing medical conditions. Sometimes advanced imaging like computed tomography, ultrasound, or magnetic resonance studies clarifies the picture before determining definitive management.
Emergency care usually involves rest through immobilisation - typically a plaster - with elevation in a sling. Raising the limb controls inflammatory swelling effectively. It's essential to remove rings from the injured hand early - as swelling develops, rings can act like tourniquets and restrict blood flow to your fingers.
Conservative treatment
Numerous fractures mend without operative intervention. The least invasive approach might involve immediate controlled movement. Others benefit from temporary external support such as splints, alongside guided exercise protocols.
Operative management
Certain fracture patterns necessitate surgical stabilisation. This can be done in one of two ways:
Closed reduction: The fracture receives manual realignment through intact skin. Maintenance of position uses either external supports (such as plaster) or k-wires (fine metallic pins) which are passed percutaneously across the break. Specialised distraction devices occasionally prove useful.
Open reduction: Surgical exposure through an incision permits visual confirmation of anatomical restoration. Fixation then employs a combinations of pins, threaded screws, or plate constructs.
Selected open injuries and occasional closed fractures benefit from external fixation apparatus - a scaffold mounted externally and anchored to bone via transcutaneous pins.
Hardware selection reflects your fracture geometry and soft tissue status. Wire fixation typically requires removal at a later date - performed either during clinic visits or with a minor secondary procedure if buried. Plates and screws sometimes need removal; I'll provide guidance specific to your case.
Post-procedure, expect immobilisation in plaster or thermoplastic splint with specific movement instructions. Your hand therapist orchestrates the rehabilitation phase.
-
Results hinge on multiple interdependent factors including your physiological healing capacity. Joint surface involvement or concomitant soft tissue injuries generally worsen prognosis. I'll talk you through expected outcomes and timelines, but exact predictions are difficult as each fracture behaves differently. How things look may change as your treatment continues.
Healing phases:
Skeletal consolidation: typically 4-6 weeks
Grip strength recovery: approximately 3-4 months
Joint mobility: initially restricted but progressively improves through activity and exercise
Longer term:
Discomfort with cold exposure, intense use, or inadvertent impacts commonly persists but gradually fades without limiting daily function. Fractures traversing articular cartilage increase risk of arthritis developing down the line. I'll clarify whether this risk applies to your specific injury.
