Finger arthritis
Understanding finger arthritis
Osteoarthritis commonly affects the fingertip joints (distal interphalangeal joints or DIPJs) and can also involve the thumb's base joint (discussed separately as basal thumb arthritis).
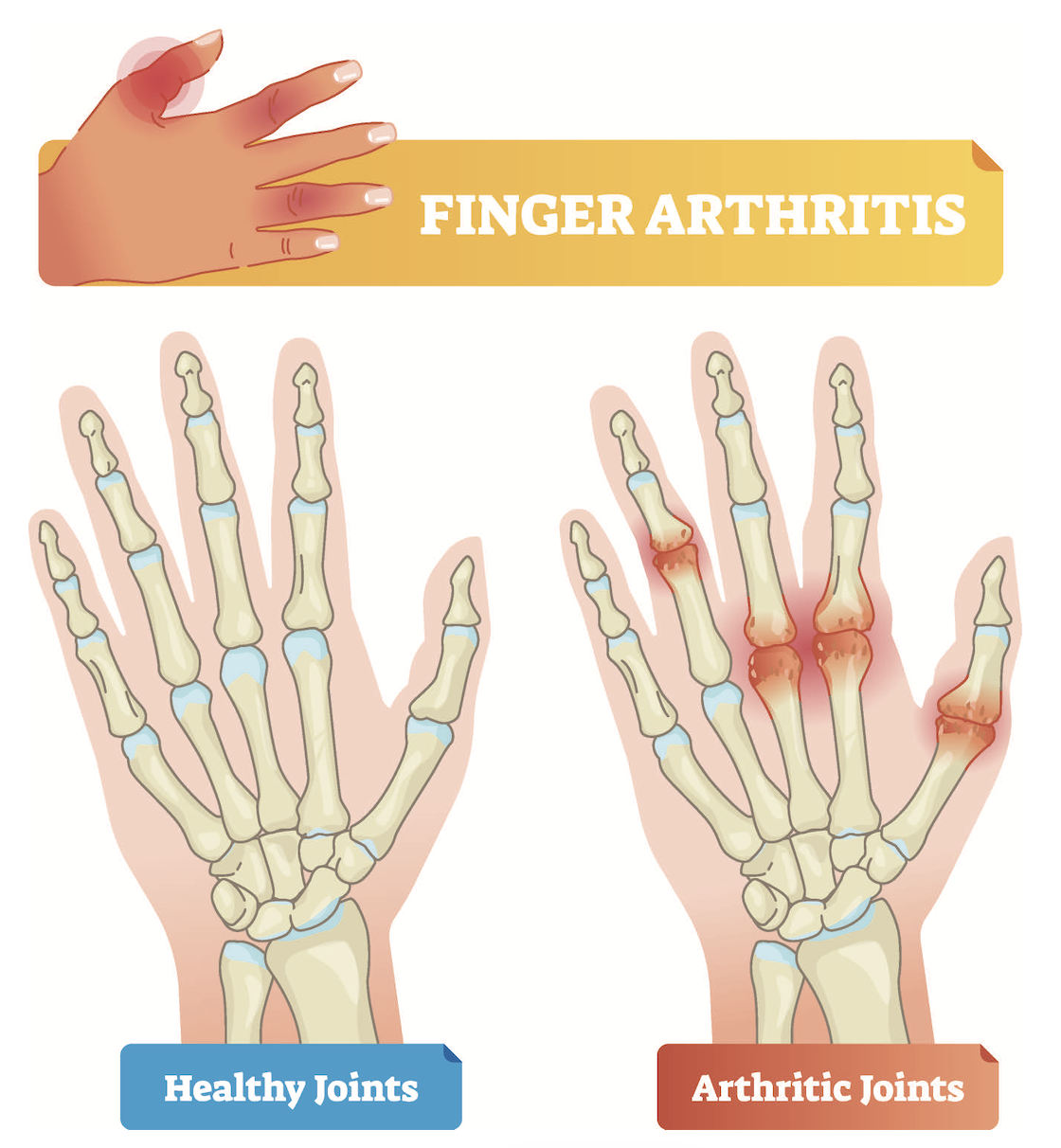
In healthy joints, smooth cartilage coats the bone ends, allowing friction-free movement. Osteoarthritis causes this cartilage to deteriorate - becoming thinned and irregular - eventually allowing bone-on-bone contact. While osteoarthritis can emerge at any age, onset typically occurs after 45 years. Genetic predisposition plays a role, with the condition often appearing across family generations.
-
Discomfort in the affected joints
Joint swelling and inflammation
Progressive deformity
Reduced range of motion
Functional limitations
Many patients develop firm nodules on the joint's back surface. These bony prominences, called osteophytes or Heberden's nodes, represent bone overgrowth characteristic of osteoarthritic changes.
Interestingly, symptom severity varies considerably and can fluctuate over time. Many individuals with radiographic evidence of advanced arthritis experience minimal discomfort. Despite visible joint enlargement and angulation, hand function often remains remarkably preserved.
-
Inflammatory flare-ups frequently subside naturally over weeks to months. During symptomatic periods, management strategies include:
Activity modification to avoid aggravating movements
Over-the-counter analgesics
Topical anti-inflammatory preparations
Oral anti-inflammatory medications
Corticosteroid injections for persistent symptoms
-
When conservative measures provide inadequate relief, surgical intervention may be appropriate.
Joint fusion (arthrodesis): this procedure permanently eliminates motion at the painful joint by fusing the bones together. The joint is typically positioned straight or with slight flexion. While fusion reliably resolves pain, the trade-off involves complete loss of movement at that joint - a decision requiring careful consideration of functional impact. Multiple surgical techniques achieve fusion. I'll explain my preferred approach for your specific situation. Post-operatively, protective splinting supports the fusion site for several weeks during bone healing.
Joint replacement (arthroplasty): flexible silicone or metal implants offer an alternative that preserves some motion. I can discuss whether you're a suitable candidate for this option and explain the associated risks and benefits.
